Skin cancer does not send a warning. It does not hurt. It does not interrupt daily life in any obvious way. What it does is sit quietly on the surface of the skin, looking like something forgettable, while the biology underneath follows its own timeline entirely independent of whether anyone has noticed. People who work outdoors on the Gold Coast for decades often discover lesions not because something alarmed them, but because a doctor spotted something during an unrelated appointment. That is not a good system. Seeing a skin cancer doctor in Gold Coast deliberately – not accidentally – is the difference between finding something manageable and finding something that has already moved.
The Overcast Day Problem
Here is something most Gold Coast residents do not know. Ultraviolet radiation penetrates cloud cover almost entirely. A fully overcast sky reduces UV by a fraction – not enough to matter. People who are careful about sun protection on bright days routinely skip it when the sky is grey and accumulate significant unprotected exposure across years of overcast mornings at the beach, on building sites, and on boats. The skin does not distinguish between sunny damage and cloudy damage. It records all of it identically. The dermal consequences of a lifetime of overcast-day exposure in this region are real, and they are seldom attributed correctly.
What Gets Missed Without Dermoscopy
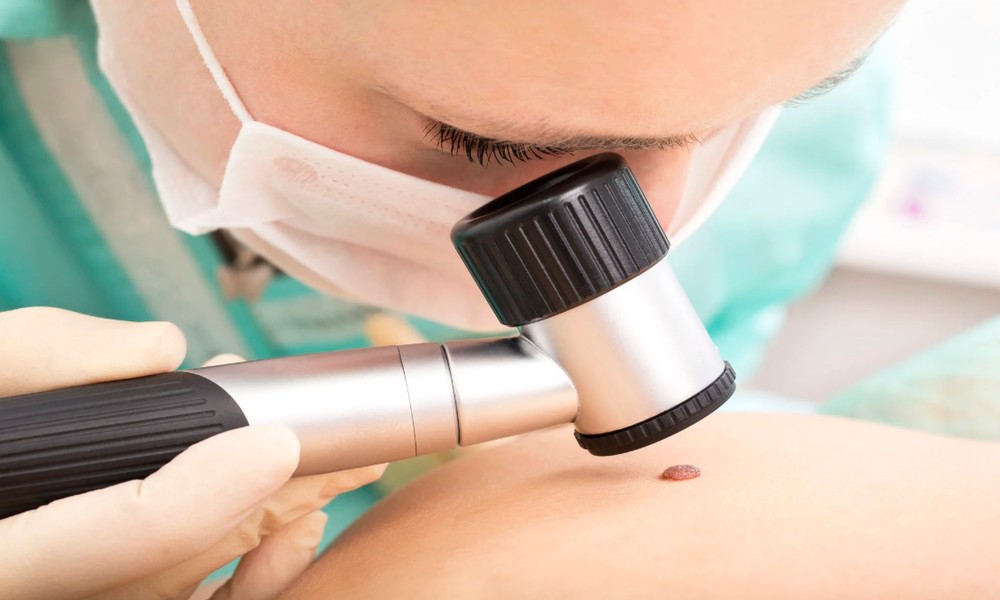
There is a specific type of melanoma – amelanotic melanoma – that contains little to no pigment. It does not present as a dark, irregular mole. It looks pink, or flesh-coloured, or like a sore that is taking too long to heal. Visually, it resembles almost nothing dangerous. Under dermoscopy, the vascular pattern it produces is distinctive and recognisable to a trained eye. This is not an obscure edge case – amelanotic melanoma is consistently among the most delayed diagnoses in skin cancer, precisely because it does not look like what people expect melanoma to look like. A skin cancer doctor in Gold Coast, using dermoscopy systematically, will catch presentations that a visual inspection would send home with reassurance.
The GP Referral Gap
General practitioners refer patients to skin cancer specialists when something looks suspicious. The problem with that model is that it relies on the GP catching the suspicious lesion first. Research within dermatological circles has documented the referral gap – the cases that were examined by a GP, assessed as benign, and later identified as malignant by a specialist. This is not a criticism of general practice. It reflects the reality that dermoscopic pattern recognition requires sustained, high-volume exposure to develop. Skin cancer specialists who examine skin exclusively, across varied presentations and demographics, develops a diagnostic sensitivity that general clinical practice does not replicate. The referral model works for obvious lesions. It is the non-obvious ones that require a specialist eye from the beginning.
Lentigo Maligna and the Waiting Game
Lentigo maligna is a form of melanoma that grows on sun-damaged skin – often on the face, neck, or scalp – and is frequently mistaken for an age spot or harmless pigmentation change. It can remain in a slow-growing, superficial phase for years before transforming into invasive melanoma. That slow phase is the window. Patients who have lentigo maligna identified and treated during that window avoid the invasive transformation entirely. Those who wait – because it looked like an age spot and seemed stable – sometimes present years later with a lesion that has already changed character. The surface appearance tells almost nothing. The history and the dermoscopic pattern tell everything.
When Family History Changes the Calculation
A personal history of melanoma increases the risk of a subsequent melanoma significantly. A first-degree relative with melanoma raises individual risk in ways that require a genuinely different monitoring approach – shorter intervals, more systematic full-body mapping, closer attention to moles that would be considered low-priority in a lower-risk patient. Most people with a relevant family history are not monitored at the frequency their risk profile warrants. They attend when convenient rather than when indicated.
Conclusion
Skin cancer caught early is largely a solvable problem. Skin cancer caught late is a different conversation entirely. The Gold Coast environment creates real, cumulative risk that does not resolve itself through good intentions. Finding a skin cancer doctor in Gold Coast who understands that risk, uses the right tools, and monitors with genuine attention to individual history is not complicated. Making the appointment before something looks obviously wrong – that part requires a deliberate decision. Most people who make it early are grateful they did not wait.